Helping your care teams optimize workflows and improve care compliance.

Creating opportunities with data and automation to improve patient access, adherence, and outcomes.
Patients rely on care teams for personalized help navigating insurance coverage, accessing affordable options, securing prior authorization approvals, and staying adherent – a massive workload to complete without technology’s help.
Our in-workflow solutions give care teams access to accurate real-time data and automated capabilities to quickly connect patients with affordability programs, deliver a better prior authorization experience, and conduct outreach at scale. With Arrive Health, care teams save time, improve affordability and time to therapy, and support medication adherence – with fewer phone calls and faxes.
Insurance Details
Confidently confirm patient eligibility with accurate data that shows patient-specific pharmacy coverage details.
Cost Transparency
Easily select best-cost medications by viewing accurate pricing information presented within the ordering workflow that shows patient-specific insured cost of care, coverage details, and discounts.
Alternatives
Avoid pursuing medications with benefit restrictions or sending scripts out of network with market-leading RTPB data that shows best-cost, non-restricted alternatives, including medication and pharmacy alternatives, and patient affordability programs.
Prior Authorization
Save time by using prospective ePA capabilities and a proprietary intelligence layer to automatically start the approval process when prior authorization is required. Keep patients informed with integrated patient status messages. The only work is answering the questionnaire.

Automated Outreach
Optimize workflows with automated capabilities that share discount card and co-pay assistance information, send proactive PA status updates, and drive adherence – while also reducing phone call/fax volumes.
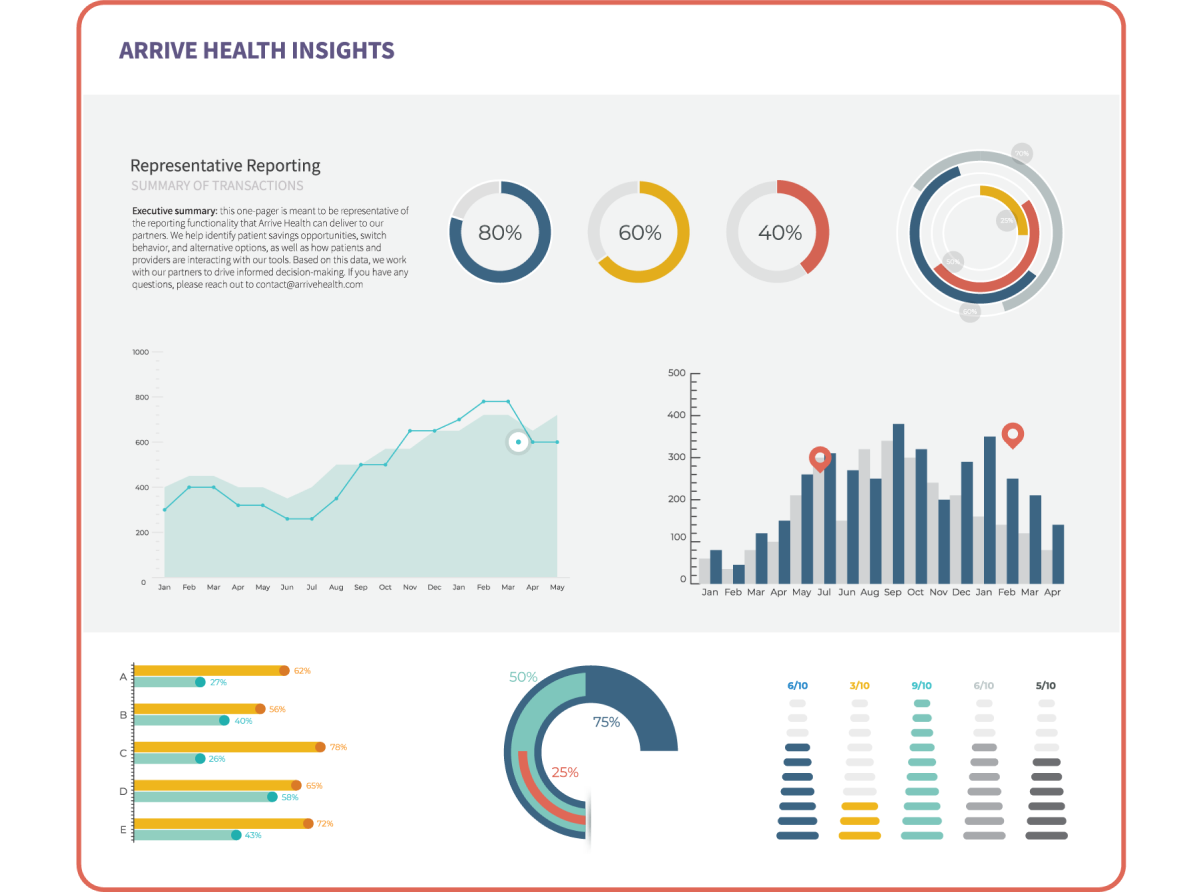
Insights
Grow impact with reports and insights that show patient savings improvements, adherence, outcomes, and patient engagement opportunities.
90%+
4-hr
$4B
Request a Demo
Find out how Arrive Health’s solutions can support your business objectives. Reach out to schedule a demo today.